Ridiculously Short Summary of What Candida Overgrowth Syndrome Is
Candida overgrowth occurs when Candida, a type of yeast normally found in small amounts in the body, grows excessively and disrupts the natural balance of bacteria and fungi. This can happen due to factors like antibiotics, high-sugar diets, weakened immunity, or hormonal imbalances. Symptoms may include digestive issues, fatigue, recurring infections, brain fog, chronic fatigue, and skin problems. It typically also interferes with the activities of the thyroid and adrenal glands (which I am not going to get into here).
What is Candizolv and how does it work?
 Candizolv is an anti-candidal product which often seems to work often with customers who claim they have “tried everything” for their candida overgrowth*** (see comments below) and nothing has worked. Individual results vary, but in some cases Candizolv works so well as to almost be bad for business! Does it work for everyone? No, in fact no product works for all the people, all of the time for anything! But it does get good results for a lot of peple (see reviews for customer comments). In the USA it sells at the riduculous price of $100 per bottle, which is equivalent to nearly £100, what with the VAT and import duty. We sell it at a more realistic price, especially at the moment whilst we have around 50 bottles on sale.
Candizolv is an anti-candidal product which often seems to work often with customers who claim they have “tried everything” for their candida overgrowth*** (see comments below) and nothing has worked. Individual results vary, but in some cases Candizolv works so well as to almost be bad for business! Does it work for everyone? No, in fact no product works for all the people, all of the time for anything! But it does get good results for a lot of peple (see reviews for customer comments). In the USA it sells at the riduculous price of $100 per bottle, which is equivalent to nearly £100, what with the VAT and import duty. We sell it at a more realistic price, especially at the moment whilst we have around 50 bottles on sale.
*** I just want to mention that in a quarter of a century I have not come across anyone who has genuinely “tried everything” for candida overgrowth syndrome, when I drill into it. The people who tell me this have on average tried half a dozen things, maybe even a dozen before getting frustrated / disheartened. A few people who say this, haven’t actually tried anything as far as I am concerned, because they dabbled with products. People who can’t be bothered to take products for more than a week or two, if they remember etc, consistently get dismal results.
Unlike probiotics and antifungal herbs which basically kill harmful fungi, bacteria, and in some cases parasites too, Candizolv works by “dissolving” candida through enzymic activity. It basically works by breaking down the outer wall of the candida cell, which then causes cellular collapse. The clever bit is that the enzymes in Candizolv break down candida, and candida only. It’s not useful against parasites or bacterial overgrowth, so you’d need other products if that’s your problem. On the positive side, it won’t attack any healthy bacteria already in your gut lining, nor will it harm any probiotics that you take at the same time. In fact it basically doesn’t have any effect, except destroying candida cell walls.
Read customer reviews of Candizolv here
A Quadruple Whammy Against Candida
Going into this a bit further, I am going to briefly discuss three other products which are typically amongst my most common recommendations. The more of them one uses, the better generally speaking, the results will be.
 Fivelac
Fivelac
This is a five strain probiotic, containing the following friendly bacteria. The information below provides detailed information which goes beyond what we publish on the web site : –
Bacillus Subtilis – an extensively studied probiotic on a genetic and functional level. There are several probiotic products in the pharmaceutical and agricultural markets that utilise this powerful probiotic. One function of Bacillus Subtilis is its ability to produce number of antibiotic compounds that are potent fighters of opportunistic and harmful bacteria. Bacillus Subtilis also produces a number of other nutrients that have systemic health benefits such as B vitamins and Vitamin K2. Bacillus Subtilis offers the important function of fighting off pathogenic bacteria and producing key nutrients in the gut itself. In addition, it is an extremely potent immune stimulator. It has the function of germinating in the small intestines to some degree and this offers the effect of broad-spectrum immune stimulation.
1 A vegetative cell is defined as a cell which is actively growing rather than forming spores
Bacillus Coagulans – A very well studied probiotic in the spore2 family that has a profound effect on inflammatory conditions such as IBS and Crohn’s. Bacillus Coagulans has the unique attribute of producing lactic acid and specifically the L+ optical isomer of lactic acid, which has been shown to have a more profound effect on immune stimulation and gut defence than the other forms of lactic acid produced by conventional probiotics. Coagulans is also a tremendous coloniser which in turn will produce the beneficial effects required. Bacillus Coagulans also plays a key role in digestion of food and absorption of nutrients.
2 A spore is a dormant type of bacterial cell. A spore can often survive for years, sometimes even decades and is only activated when it comes into contact with the right conditions for its proliferation.
Enterococcus Faecalis – A spherical bacteria that is part of the normal flora of humans. In fact, according to Todar’s Online Textbook of Bacteriology, Entercoccus Faecalis is commonly found in the vaginal and intestinal regions of about 40 to 80 percent of individuals. Apart from humans and animals, this bacteria can also be found in the soil and water. This probiotic is the source of some claims that Fivelac is “dangerous”. However this is in essence nonsense put out by competitors who seek to scaremonger. While some strains of Enterococcus Faecalis can cause opportunistic and hospital-acquired infections in humans, many other strains have been used for a variety of beneficial purposes by both nature and man.
Along with other bacteria that are part of the normal flora, Enterococcus Faecalis prevents the colonisation of pathogenic bacteria in the body of its host by competing with the pathogens for binding sites and nutrients. They may also prime the immune system by inducing the production of low levels of antibodies against its own components which in turn makes the immune system more efficient.
Strains of Enterococcus Faecalis play an important role in the dairy industry and occur in a variety of cheeses, whey and natural milk. They are more commonly used in southern Europe and help in the development of the flavour of the cheese and can also be used as cheese starter cultures. As per a June 2003 article in the International Journal of Food Microbiology, Entercoccus Faecalis also produces a compound known as bacteriocin that can prevent the growth of several other bacteria such as Listeria Monocytogenes, Staphylococcus Aureus and Vibrio Cholerae, thereby preventing the spoilage of dairy products.
Lactobacilli and Bifidobacterium – These are extra probiotics found in Fivelac that are not found in the earlier and still very popular and successful Threelac.
From https://www.ncbi.nlm.nih.gov/pubmed/10941602…
Bifidobacteria and Lactobacilli are Gram-positive lactic acid-producing bacteria constituting a major part of the intestinal microflora in humans and other mammals. Administration of antimicrobial agents may cause disturbances in the ecological balance of the gastrointestinal microflora with several unwanted effects such as colonization by potential pathogens. To maintain or reestablish the balance in the flora, supplements of intestinal microorganisms, mainly bifidobacteria and lactobacilli, sometimes called probiotics, have been successfully used. This article reviews the role of Bifidobacteria and Lactobacilli in human health.
Lactobacillus and Bifidobacterium contain a large number of species and strains, so both terms are actually general terms covering a considerable number of related bacteria. Interestingly, every company selling different strains of Lactobacillus and Bifidobacterium insist that the ones in their probiotic is officially proven to be the best one. I have a slightly more realistic viewpoint, which is that the best one is simply the one that works best for you.
You can purchase Fivelac here
View our article Threelac vs Fivelac here
A few Customer comments on Fivelac
Great gut-flora support supplement. Stable at room temperature – so much better for me than the Mightydophilus supplement I was taking before (which has to be stored in the fridge). I’m using it as part of an anti-candida regime, and feel so much healthier than I did before, and truly believe this is part of the reason for improvement.
I have been using the services of Finchley Clinic for more than ten years. I have found them to be impeccable in every way. In particular I have used Fivelac, originally Threelac before Fivelac came along, and oxygen products, at present the Fivelac. I find it absolutely invaluable for establishing and maintaining microbiome balance. Thank you Finchley Clinic!
My wife was cured of a candida infection in her digestive system (medium to high intensity) that she has been fighting with for 10 years. She’s got the condition after a herpes zoster infection and nothing has helped her. She had kept a strict diet with no sugars, no fermented staff, and so on, which alleviated a little the symptoms, but never got rid of them. After a thorough research I discovered fivelac and the more I was reading about the way it works, we became convinced to give it a try. So we did, we bought the 6 box offer and she took 2 sachets per day, one in the morning and one in the evening till all the 6 boxes had been finished. There are more than 5 and a half years since she had the fivelac and no signs of candida infections have reappeared.
I cannot recommend Fivelac highly enough. I suffered for years with systemic candida which resulted in great vulval & urinary pain/discomfort. I had endless visits to my local Genito-urinary clinic & whilst the prescribed medication eased the symptoms of thrush, no medical professional could help with all my other symptoms. I saw many specialists without result so started to research to help myself……..so discovered threelac which worked. And I simply upped it to Fivelac as more of the good bacteria could only do good. The only downside I found was constipation (I do not know if it was definitely caused by the product) which is when I started using the oxy colon cleanse products. If you suffer from constant candida, I would thoroughly recommend Fivelac.
Within 24 hours of taking Fivelac and going on the candida diet the depression in my brain cleared.
Finchley Clinic Editorial note: We contacted this customer to check what she was saying was accurate, as it’s very rare for anyone to respond that fast. She said was very sensitive, and tended to react very quickly to products. She said it was true, she had taken 3 sachets per day, and started noticing the benefits on the second day. She said she was not completely cured, but there was a big improvement. She attributed this improvement mostly to Fivelac.
Thyme Formula
Please note, we recommend that this product is taken away from probiotics by an hour or more. We suggest taking one of them with meals, and the other one away from meals in order to separate them. It doesn’t really matter which way around you do it. And by the way, Candizolv (above) can be taken with anything, with or away from food.
Thyme Formula doesn’t have as pretty a label as the products made by our bigger suppliers. Nor will you find lots of companies selling it. What it does do, is work! It contains seven herbs all of which are anti-candidal in their own right, but blended synergistically, they are much more powerful than one herb in seven times larger amounts. As the product developer explained…
These formulae have been developed because we were dissatisfied with currently available products. Using our test system (Vega Biokinesiology), we find that single herbs “power score” (a measure of efficacy) 5-20, currently available herbal formulae power score 15-30, and our formulae power score 35-50. We therefore believe that our formulae are up to three times more effective than existing herbal formulae.*
The herbs used in our formulae have been selected purely empirically, without recourse to the literature. For each formula we screen hundreds of herbs and then having made the initial choice we test for antagonism, synergism, allergenicity and tolerability before we decide on the final selection. In all we conduct around three thousand separate tests for each formula.
Clinical experience has quickly confirmed the validity of our system and we now have numerous testimonials and case-histories to demonstrate the efficacy and safety of our range.
It contains the following benefits for candida sufferers : –
1. Thyme Formula is a highly effective herbal remedy, which brings Candida under control in 2-3 months, and usually eliminates it within six months. {Note it is not like a paracetamol, designed to give symptomatic relief in 30 minutes}. One bottle is 2 weeks supply on the typical full label dosage. Sensitive individuals may need to take a lower dosage, which means the bottle will last longer.
2. Thyme Formula has been designed to penetrate all organs including those difficult to access, e.g. colon, brain, vagina, and bone.
3. Thyme Formula contains several different anticandidal herbs and therefore possesses a broader spectrum of activity than a single agent against the many different candida strains encountered clinically. For the same reason, resistance to Thyme Formula is less likely to develop. By using a combination of herbs, the ingredients work synergistically. In other words the whole is greater than the sum of the parts.
4. Thyme Formula provides an array at beneficial effects in addition to its anticandidal activity that are relevant to the control of candidiasis:
i) It supports the immune system. If Candida is merely killed by an antifungal agent and the immune system left unsupported, the chances of recurrence are high.
ii) It supports the liver, which is usually stressed by Candida and its toxins. Improving liver function helps combat Candida overgrowth since the liver is part of the immune system, and since bile is inhibitory to intestinal Candida. The liver is also the main eliminatory organ for Candida toxins, which cause many of the symptoms associated with candidiasis.
iii) It enhances secretions from all digestive organs. Such secretions inhibit intestinal Candida and diminish gas production, a frequent problem in candidiasis.
iv) It supports the adrenal glands. There is a reciprocal relationship between the adrenal glands and Candida: hypofunction of the adrenal glands permits Candida overgrowth, and Candida damages the adrenal glands by free-radical and autoimmune mechanisms.
v) It helps treat intestinal bacterial dysbiosis. Dysbiosis is responsible for allowing Candida to overgrow in the first place, and additionally, contributes to the intestinal disturbance (gas, bloating, and discomfort) and systemic toxicity associated with candidiasis.
vi) It helps heal the leaky gut induced by Candida. A leaky gut encourages the development of food allergies and facilitates the absorption of toxins from the bowel.
vii) It is strongly anti-protozoal. Infestation with intestinal protozoan parasites such as Giardia and Blastocystis often accompanies candidiasis. Such a parasitosis may cause some of the symptoms attributed to Candida (gas, bloating, constipation, diarrhoea, leaky gut, dizziness, fatigue), and may also give rise to immunosuppression.
viii) It possesses useful anti-nematode activity. Nematode (worm) infestation sometimes accompanies candidiasis and may be responsible for some of the symptoms attributed to Candida (abdominal discomfort gas, ileo-caecal valve dysfunction, leaky gut, fatigue), and may also give rise to immunosuppression.
ix) It helps treat the hypoglycaemia that often results from candidiasis. Much of the malaise and discomfort experienced by Candida victims originates from hypoglycaemia.
You can read our customer reviews for Thyme Formula here. For those who tend to get habituated to herbal products so that they work to begin with, then tend to stop working, it can (and should) be alternated every couple of weeks with its sister product, Oregano Formula. Another popular, though more expensive alternative is Global Healing’s Candida Balance. This can also be used as an alterative to Thyme Formula and Oregano Formula, or alternated with them, especially in stubborn cases.
The fourth element of the Quadruple Whammy: Dealing with Candida Toxins / Candida Die-Off
Candida die-off, or a Herxheimer reaction, occurs when anticandidal treatments rapidly kill Candida yeast, releasing toxins into the body. This sudden toxin release can overwhelm detox pathways, causing symptoms like fatigue, headaches, brain fog, nausea, bloating, skin rashes, and flu-like feelings. Some may also experience irritability and anxiety, or dizziness. These symptoms typically begin within a few days of starting strong anti-Candida products and may last from a few days to many weeks. It’s the main cause of some people contacting us to say they can’t tolerate the types of products described above. Candida toxins also cause free radical damage, so in my opinion should be avoided, and not “put up with” as a short term annoyance or welcomed as “proof the products are doing something”, even though some people do have that (wrong) attitude.
 My favourite product for mitigating this is Wild Endive Formula, or the extremely similar Wild Endive Formula A (for those who are sensitive to ginger or cannot tolerate the very mild anticandidal effects of Wild Endive Formula, as the “A” formula has no anti candida action at all). This product was formulated specifically for candidal toxins (not eliminating candida itself), though doubtless it also helps with bacterial toxins, parasite toxins, etc. Severe candida sufferers should consider getting the large 5 bottle sizes of either of these products, as some people need to take high dosages, or take it for quite a long time.
My favourite product for mitigating this is Wild Endive Formula, or the extremely similar Wild Endive Formula A (for those who are sensitive to ginger or cannot tolerate the very mild anticandidal effects of Wild Endive Formula, as the “A” formula has no anti candida action at all). This product was formulated specifically for candidal toxins (not eliminating candida itself), though doubtless it also helps with bacterial toxins, parasite toxins, etc. Severe candida sufferers should consider getting the large 5 bottle sizes of either of these products, as some people need to take high dosages, or take it for quite a long time.
For those who prefer to use a liquid rather than capsules, I usually recommend Manayupa-Pinella (blood / kidney / liver / brain detox). Another alternative to Wild Endive Formula is Global Healing’s Liver Health, which has also proven very popular over the years.
This is not a comprehensive article on candida die-off, or for that matter on candida itself. I can’t really do that in a single newsletter (it would take a whole book to cover the subect in full). But I have squeezed in as much as possible into a less than 10 minute read.

Best Wishes
Mark G. Lester
Director / Founder
(aka Captain Candida Crusher)
The Finchley Clinic Ltd
www.thefinchleyclinic.com
www.thefinchleyclinic.com
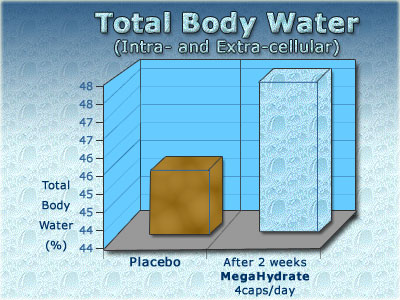 MegaHydrate and Crystal Energy
MegaHydrate and Crystal Energy
 Hope this helps, and thank you for attention.
Hope this helps, and thank you for attention.  Fivelac
Fivelac
 Keywords: Detoxification, Colon Cleasing, Colonic Irrigation, Constipation, Disease Prevention, Overall Health
Keywords: Detoxification, Colon Cleasing, Colonic Irrigation, Constipation, Disease Prevention, Overall Health The colon a.k.a large intestine, is bascally the long loopy thing at the end of the digestive tract, who’s role it is to absorb water (but not too much, otherwise constipation occurs) and electrolytes (which balance the amount of water in your body), collect and form waste (also known as “poop”) into the right consistency in preparation for elimination (in other words being pooped out). It’s also one of the most common organs to not function well, due to poor diet, stress, innate tendency (in some people), suboptimal liver (and perhaps kidney) function, improper lifestyle (in other words, most of us), and doubtless other reasons that don’t come immediately to mind. Being constipated is particularly bad for us, as having gunk swishing about in our guts means there is an unhealthy contact time between carcinogens, bacteria, fungi and other toxins from our diet with the gastrointestinal tract, giving those harmful substances more time to do their mischief. Not good!
The colon a.k.a large intestine, is bascally the long loopy thing at the end of the digestive tract, who’s role it is to absorb water (but not too much, otherwise constipation occurs) and electrolytes (which balance the amount of water in your body), collect and form waste (also known as “poop”) into the right consistency in preparation for elimination (in other words being pooped out). It’s also one of the most common organs to not function well, due to poor diet, stress, innate tendency (in some people), suboptimal liver (and perhaps kidney) function, improper lifestyle (in other words, most of us), and doubtless other reasons that don’t come immediately to mind. Being constipated is particularly bad for us, as having gunk swishing about in our guts means there is an unhealthy contact time between carcinogens, bacteria, fungi and other toxins from our diet with the gastrointestinal tract, giving those harmful substances more time to do their mischief. Not good!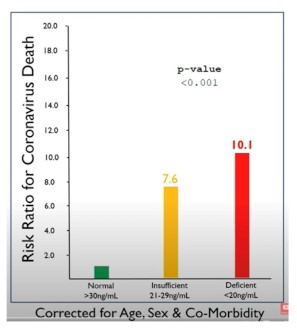 Vitamin D and viral illness (colds, flu’s & covid)
Vitamin D and viral illness (colds, flu’s & covid) Wishing You All An Abundant Viral Free Life
Wishing You All An Abundant Viral Free Life